When ‘healthy’ isn’t always clear: Making sense of nutrition in a crowded information environment
A survey of 1,500 US adults shows how some Americans navigate nutrition advice today—and points to where simpler signals and better tools could help support healthier choices
Eating healthy can feel like guesswork. Nutrition science often evolves, and recommendations can be complex. What’s healthy for one group, like college athletes, may be different from what’s healthy for another, like older adults.
Adding to this dynamic, Americans can encounter different advice shaped by science, fad diet trends, and a high-volume commercial information environment. This includes nearly $14 billion a year in food industry advertising, which can influence health expectations and norms.1 Additionally, half of Americans say they have encountered food and nutrition content on social media in the past year, according to the 2025 International Food Information Council Food and Health Survey of US adults.2
Current federal priorities focus on improving healthy diets through a whole-of-government approach to confronting America’s chronic disease crisis, with key reforms aiming to develop a uniform definition of ultra-processed foods, reform dietary guidelines, and strengthen nutrition research and education.3 States and localities have also been exploring ways to integrate nutrition into health care, expand education, and help patients, families, and communities access healthy foods.4
Helping Americans make healthier food choices involves an understanding of not just what they know about healthy eating, but also what they think they know. It also means examining how habits, preferences, and today’s information ecosystem shape those perceptions.
To explore these dynamics, Deloitte’s Center for Government Insights conducted a nationally representative survey of 1,500 US adults in October 2025 using an online panel matched to US census categories (see methodology). The results show that while Americans want to make healthy choices, they face conflicting information and often rely on gut instinct, nutrition labels, and perceived health benefits to decide what counts as healthy. They want both simple decision-making tools, like expanded nutrition labels, and deeper resources explaining the science behind nutrition guidance to support healthier choices. Findings highlight opportunities for government and industry to use clear guidance, digital tools, and educational campaigns to meet Americans where they are.
Many Americans decide what’s healthy based in part on “gut” feelings, but they aren’t always making healthy choices
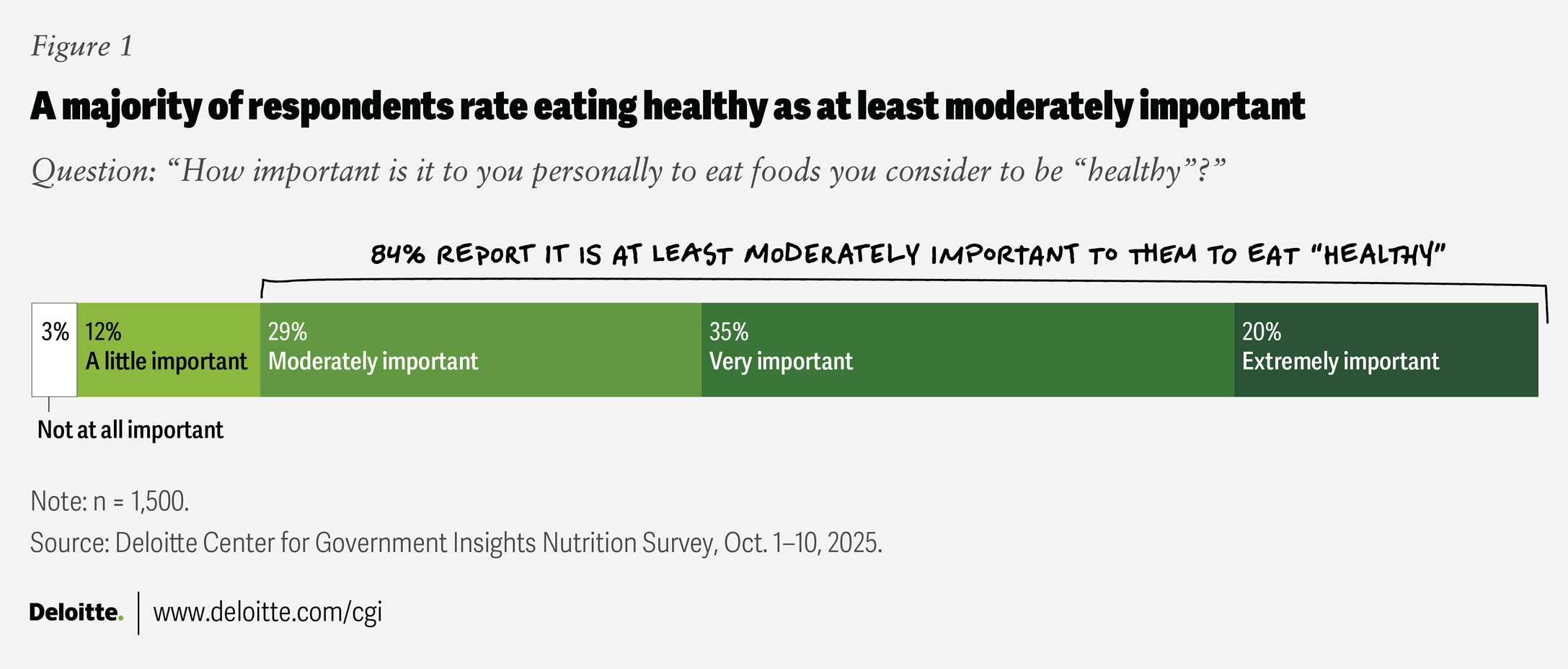
Healthy eating today appears to be an American priority: Eighty-four percent of respondents report that healthy eating is important to them, with more than half ranking it as very or extremely important (figure 1). Another 12% say healthy eating is only a little important, while just 3% report that it is not at all important.
Despite this prioritization of healthy eating, most respondents report that they do not follow ideal diets. Only 30% say their diets are very closely or completely aligned with their perception of ideal eating habits. A plurality report that their diets are only somewhat aligned with their ideal eating habits (figure 2).

Existing research suggests that multiple ecosystem factors contribute to the gap between actual and optimal diets. Cost concerns,5 limited time to shop and cook,6 differences in access to healthy foods across neighborhoods and demographics,7 ingrained unhealthy habits,8 and the appeal of highly processed, calorie-dense foods all shape whether Americans make healthy food choices.9
Our survey sheds light on another part of the story: how people decide what counts as “healthy” in the first place and the criteria they rely on to make that judgment. While prior research has focused on external cues in deciding what’s healthy,10 our survey adds to the literature by capturing a novel application of internal, subjective judgment as a cue for perceived healthfulness, alongside more conventional criteria.
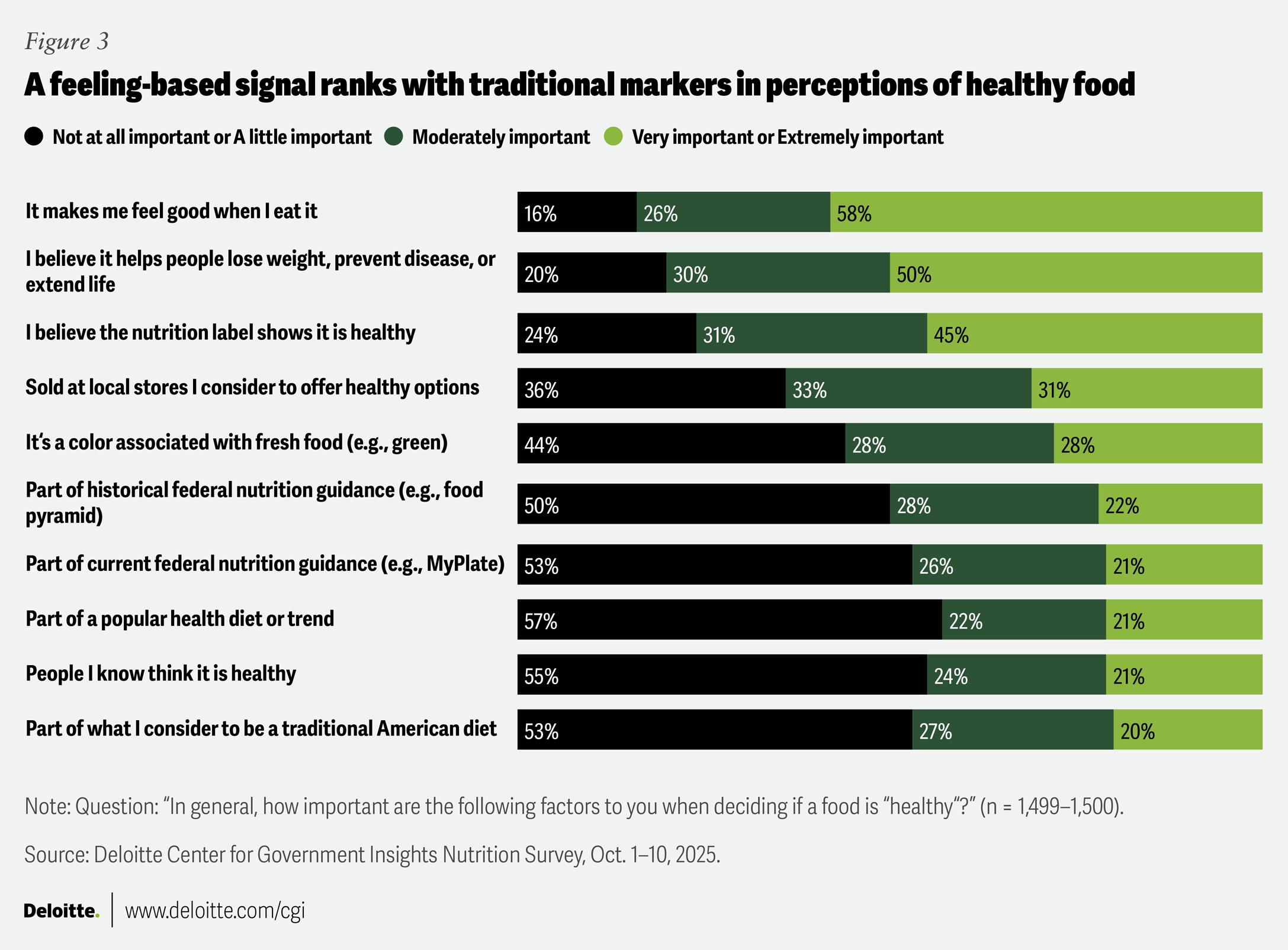
When asked how important different factors are in deciding if a food is healthy, “It makes me feel good when I eat it” was the top criterion: Fifty-eight percent said it was very or extremely important, while only 16% said it was of little or no importance (figure 3). The meaning of “feeling good” may vary across respondents, ranging from a sense of well-being or reassurance to simple enjoyment while eating. Outcome- and information-based measures ranked close behind, with half of respondents prioritizing weight loss, disease prevention, or longevity, and 45% pointing to nutrition labels (figure 3).
These findings suggest that internal, feelings-based judgments can play a prominent role in how people define healthy foods, alongside more objective signals, underscoring the complexity of these decisions.
Conflicting nutritional information can overwhelm decision-making
Breaking old eating habits can be an uphill battle, especially in a nutrition ecosystem with conflicting information, pervasive marketing, and the easy availability of convenience foods.
Our survey finds that information about what to eat and what to avoid appears to be nearly everywhere in today’s media environment. In the past year, 3 out of 4 respondents say they have passively encountered messages about how certain foods or drinks affect health at least some of the time.
These messages aren’t always in agreement with what’s healthy to eat. According to our survey, the vast majority of respondents say they have seen or heard conflicting information in the past year about how much, what, how often, and when to eat (figure 4). Conflicting recommendations about what to eat were especially common: Forty percent report hearing or seeing them often or very often in the past year, while only 8% report never coming across any.
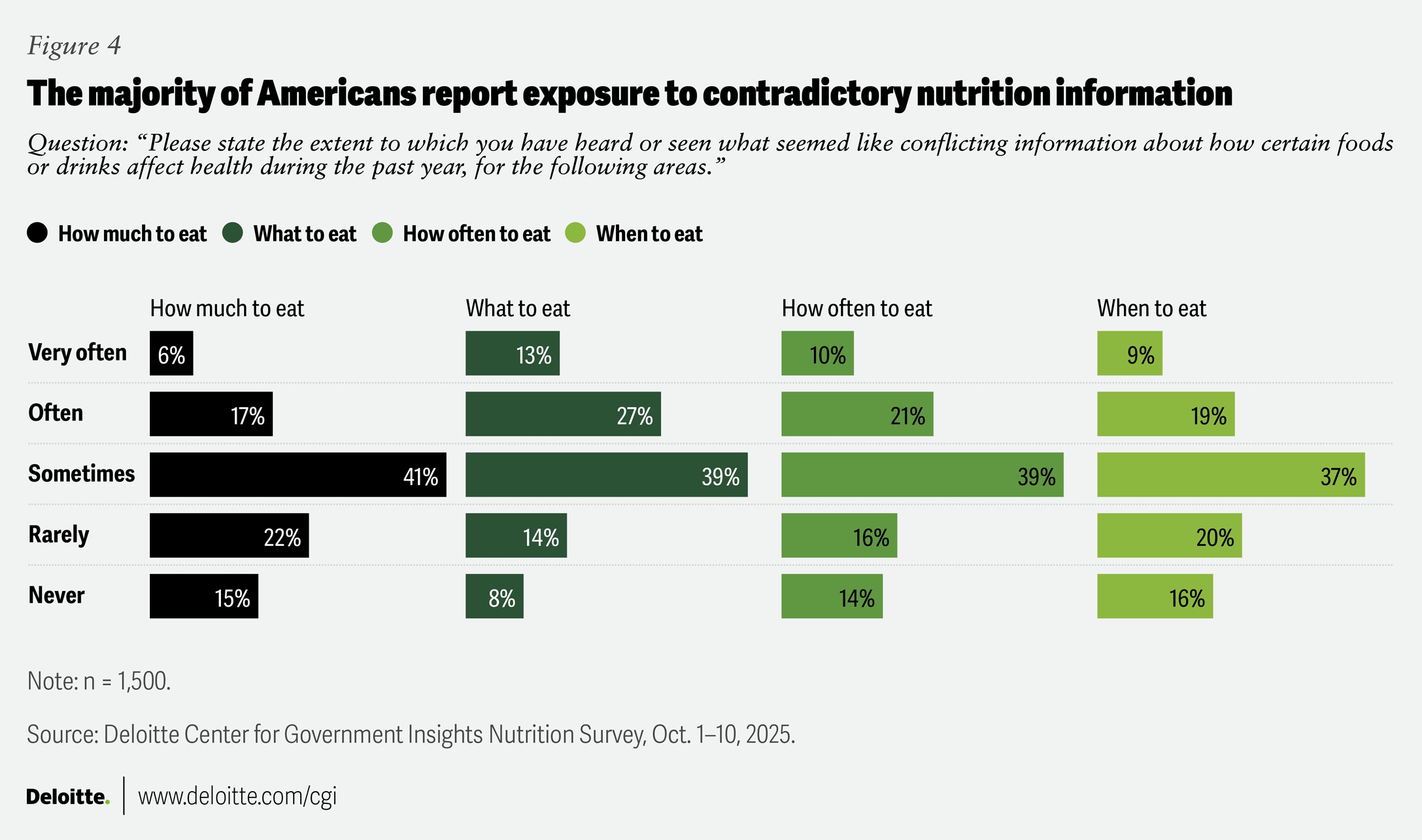
Nearly two-thirds (63%) of respondents reported feeling confused about making the best food choices for their health when faced with seemingly conflicting messages. Just 13% said they never felt confused by conflicting nutritional information (figure 5).
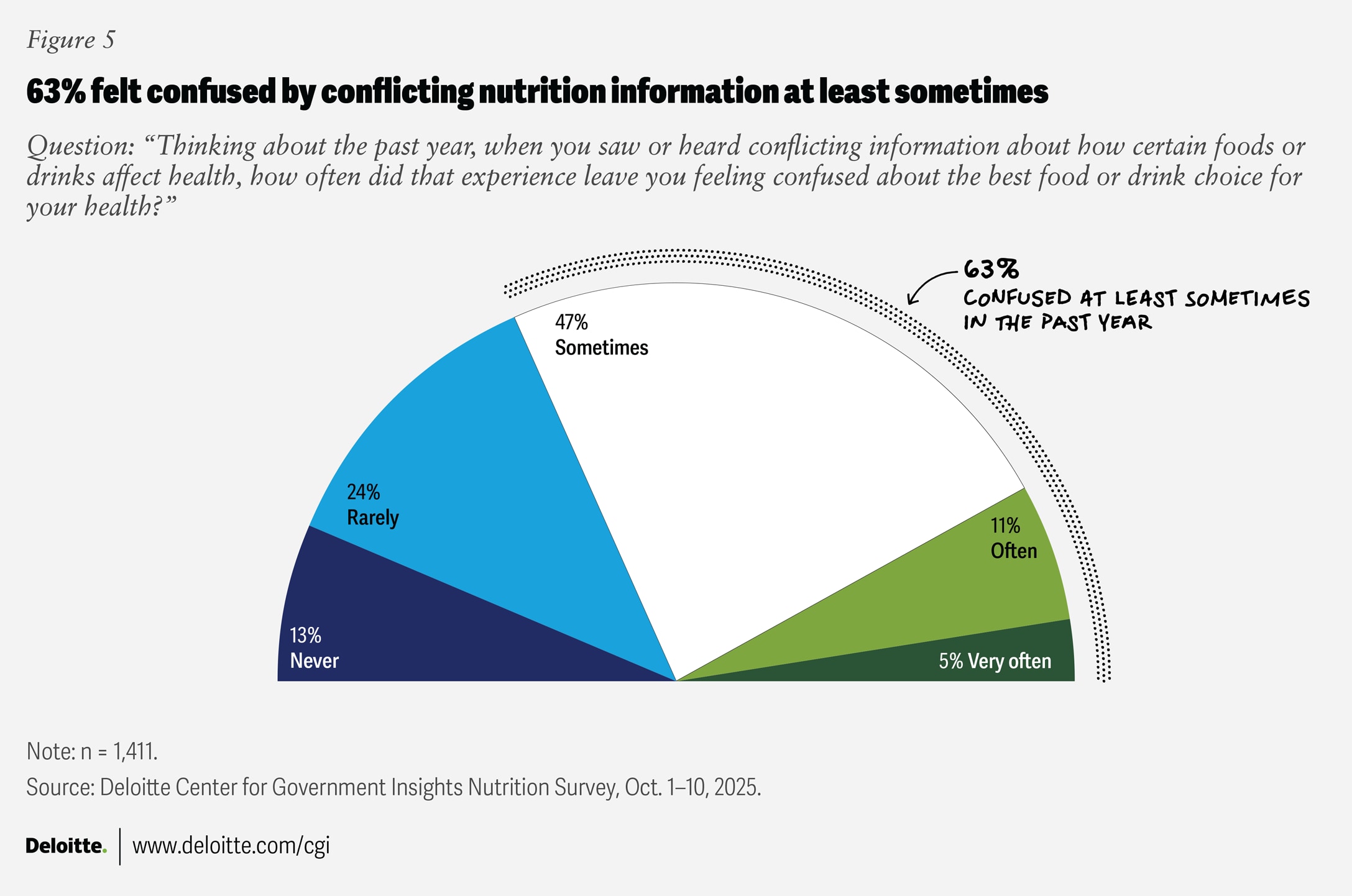
Chi-square testing shows a significant association between respondents’ views of how ideal their diets are and how confused they feel about what foods to eat for health, with confusion rising as diets drift further from what respondents consider ideal.11 One notable exception is respondents who self-identify their diets as optimal. This group is more likely to report either high uncertainty or a strong sense that they know what’s healthy, compared to those with not very, somewhat, or mostly optimal diets.12 This pattern highlights how complicated nutrition information can be to interpret, even among the healthiest eaters.
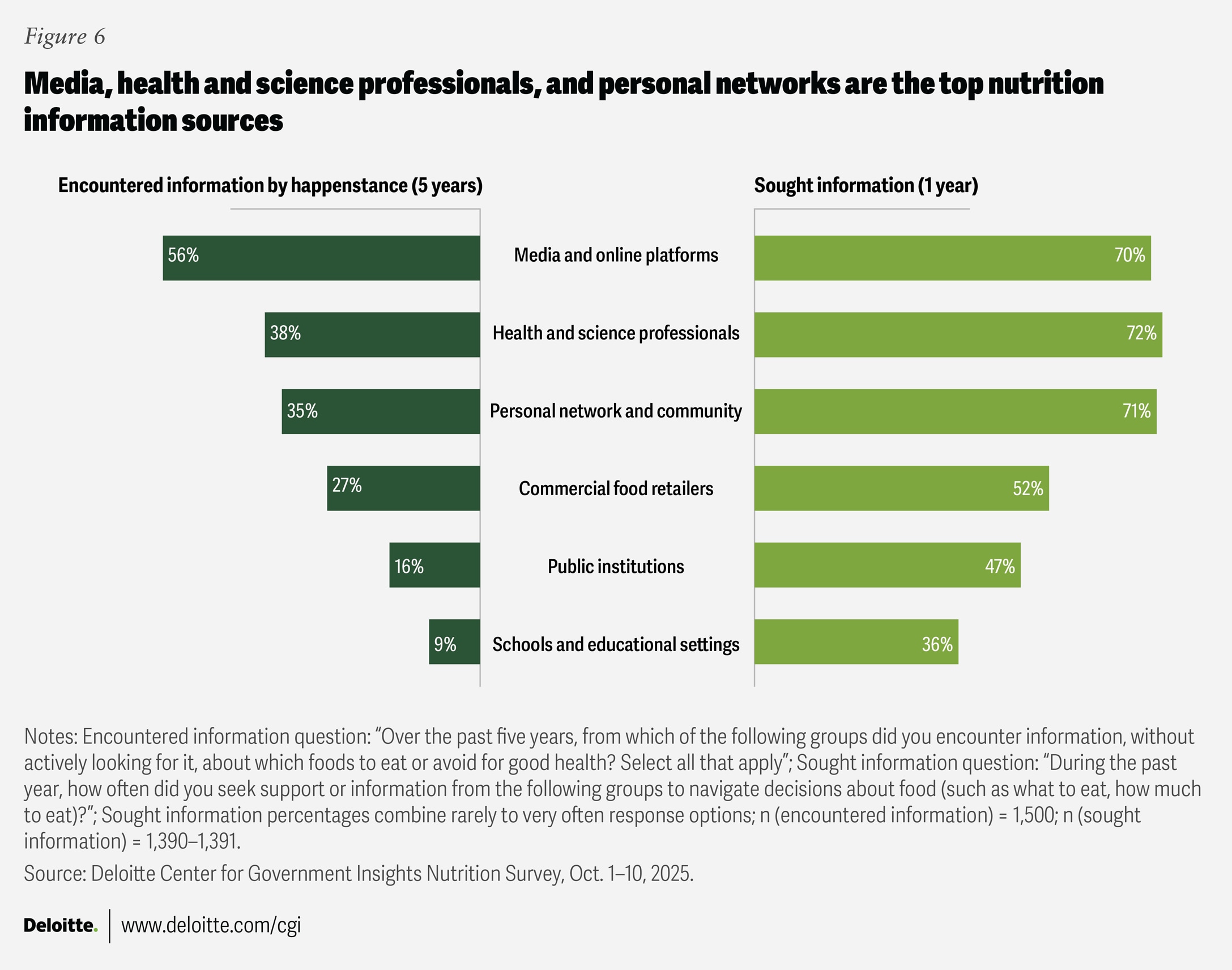
Americans receive information about which foods to eat or avoid from a wide array of sources—even when they are not actively seeking it. Media and online platforms are the most commonly cited sources of passive information, with more than half (56%) of respondents encountering nutritional information through these channels over the past five years (figure 6). This suggests that Americans learn about healthy eating through media exposure, which may, in turn, influence their dietary choices.
When actively seeking nutritional information, approximately 70% of Americans report turning to health professionals, personal networks, and the media in the past year (figure 6). Notably, public institutions and schools rarely serve as sources of passive information (16% and 9%, respectively), but they see three to four times higher rates of active information-seeking (47% and 36%), indicating more deliberate consultation (figure 6).
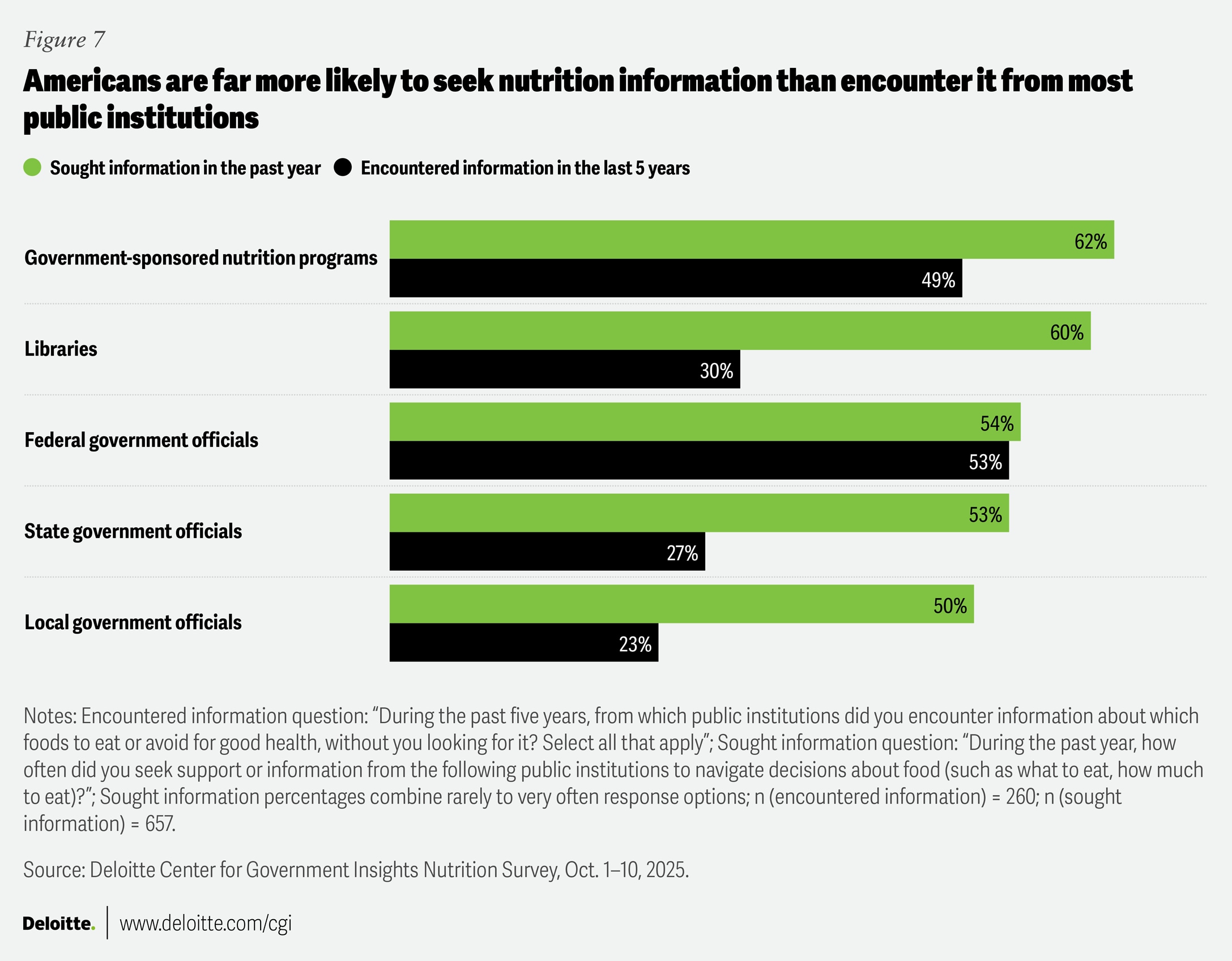
Among respondents seeking information from public institutions, government-sponsored nutrition programs (62%) and libraries (60%) top the list, with around half seeking information from federal, state, or local government sources (figure 7).
Respondents sought information from local and state governments and libraries at two times the rate at which they encountered information from those sources. This suggests a potential opportunity at the community and state levels to deliver guidance at key “moments of search,” when individuals may be most receptive to actionable nutrition information.
In an environment that includes conflicting messages, persuasive marketing, and cues toward convenience, knowing where and how to break default habits and make healthier choices can be challenging.
Many Americans we surveyed express concern about the health effects of processed foods, but struggle to identify them
For decades, the healthfulness of foods was judged largely by nutrient content, such as calories, fat, vitamins, and minerals. More recently, nutrition researchers have studied how food processing may also affect the healthfulness of foods.13 A review of 45 meta-analyses found consistent associations between consumption of ultra-processed foods, in particular, and a range of adverse health outcomes, with the strongest evidence for type 2 diabetes, although the studies were observational.14 With no single, standard definition of processing levels, even researchers disagree about how specific foods should be classified.15
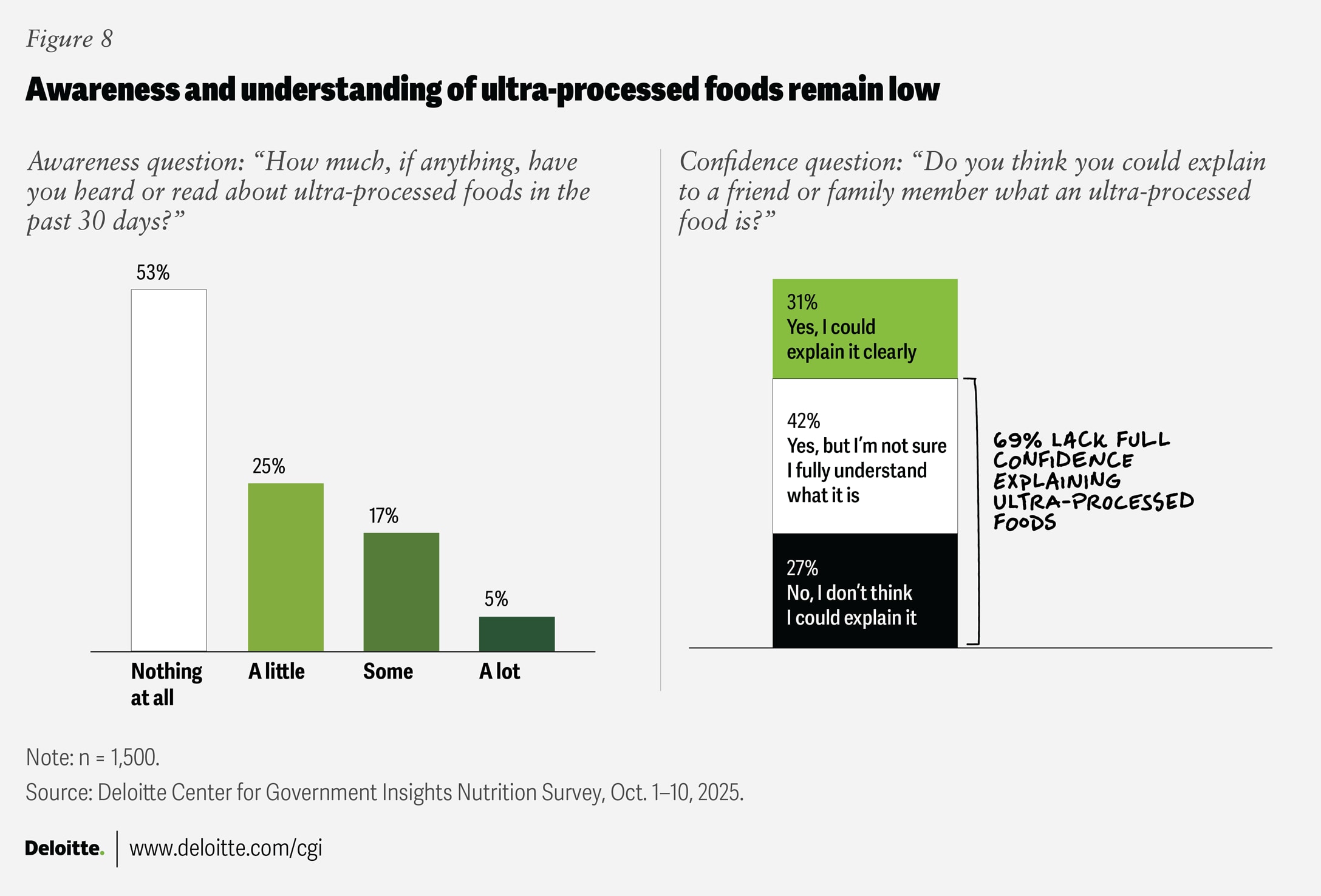
Survey findings suggest many Americans also view ultra-processed foods as less healthy than unprocessed foods, but are uncertain about which foods qualify as ultra-processed foods. Sixty-eight percent of respondents rated ultra-processed foods as worse for health, 7% as better, 13% as neither better nor worse, and 12% were unsure. Despite this perception, confidence in understanding ultra-processed foods is low: Forty-two percent were unsure they fully understood what ultra-processed foods are, 27% said they could not explain ultra-processed foods at all, and only 31% felt they could clearly explain ultra-processed foods to others (figure 8). Overall, more than two-thirds of respondents (69%) lacked confidence in their ability to explain ultra-processed foods to others.
Awareness of ultra-processed foods also remains limited, even in an environment with an abundance of nutrition information. In the 30 days prior to the survey, 53% reported hearing nothing at all about ultra-processed foods, 25% heard a little, 17% heard some, and only 5% heard a lot (figure 8).
To explore how people understand food processing in practice, we asked respondents to identify the processing levels of six carrot-based foods. Their answers drive home how hard it is to distinguish processing levels in the absence of commonly known or agreed-upon definitions.
Curious how your perceptions of processing definitions compare with respondents’? Answer the survey question yourself below, or skip to the results to find out how others answered. As you’ll see, since recognized definitions of food processing don't always align perfectly, some foods could even be classified into more than one processing category.
Rate the following carrot foods based on how processed you consider them to be
Click one option per carrot food, classifying each as unprocessed, processed, or ultra-processed
| Product | Unprocessed | Processed | Ultra-processed |
|---|
Results
Your selections are marked with a check. The percentages represent survey respondents’ choices for the given processing level. The green shading indicates what could be considered the processing level (or levels) given existing nutrition definitions (see notes).
| Product | Unprocessed | Processed | Ultra-processed |
|---|
If you found this survey question confusing, you’re not alone. Respondents had a hard time distinguishing between processed and ultra-processed foods in particular.
Even for a food like store-bought carrot cake, 54% identified it as ultra-processed, while 40% classified it as processed, effectively collapsing the two categories. Canned carrots were most often identified as processed, but a sizable share classified them as ultra-processed. Respondents were split on whether bagged baby carrots are processed or unprocessed, potentially reflecting uncertainty about the contribution of packaging and peeling to processing. Labels also influenced perceptions: When bagged carrots were labeled “organic,” they were more likely to be rated as unprocessed.
The results suggest that uncertainty about food processing isn’t just a knowledge gap but reflects the fact that processing is often defined in different ways and that health effects don’t always map cleanly onto a single category.16
Most surveyed Americans value clear, actionable nutrition guidance and labels
Our survey findings help identify where Americans appear to be stuck—and what resources could increase understanding and potentially shift behaviors.
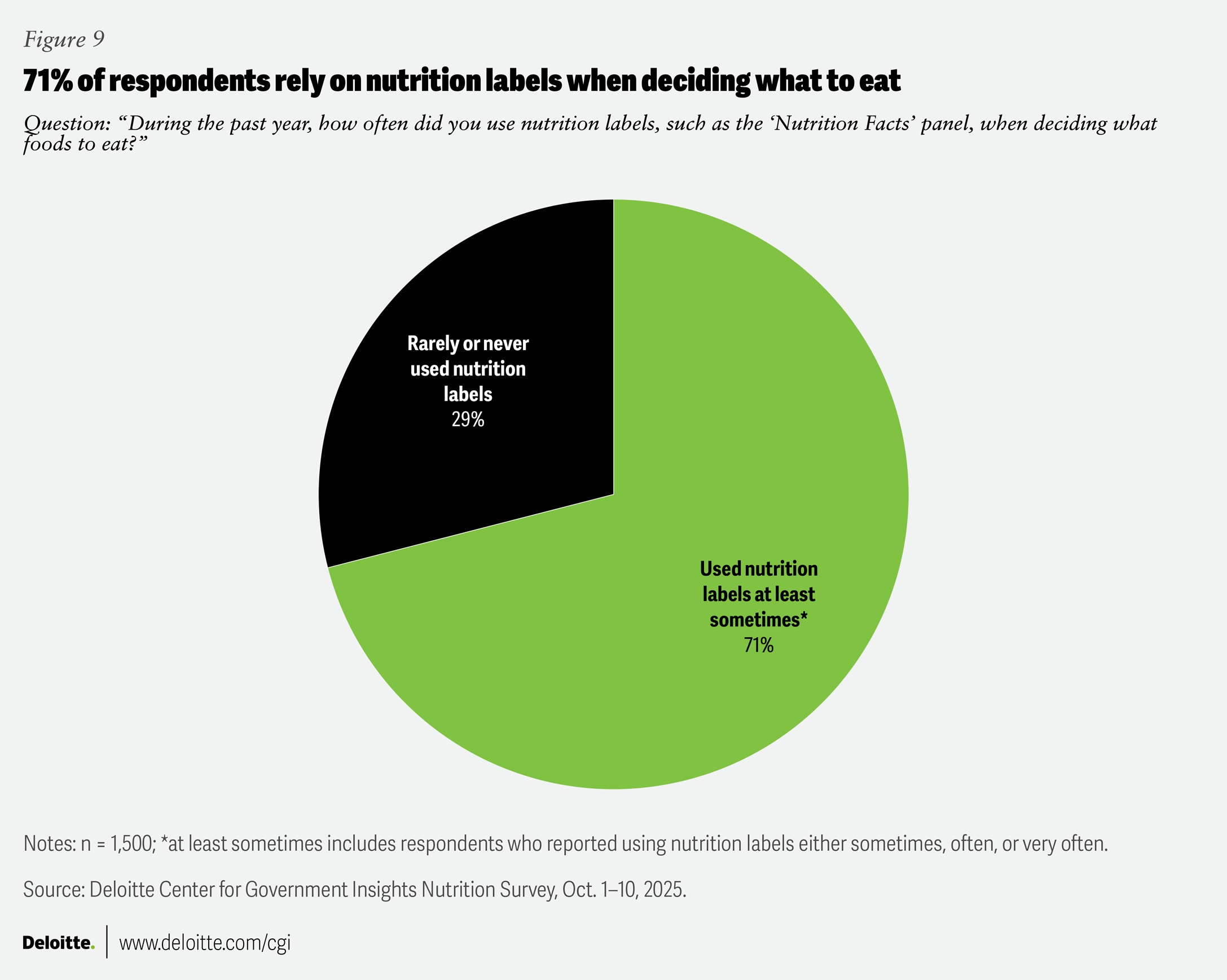
Nutrition labels serve as many Americans’ primary source of nutrition information at the point of purchase. In our survey, 71% of respondents say they use nutrition labels at least sometimes when deciding what to eat, while 29% report rarely or never using them (figure 9).
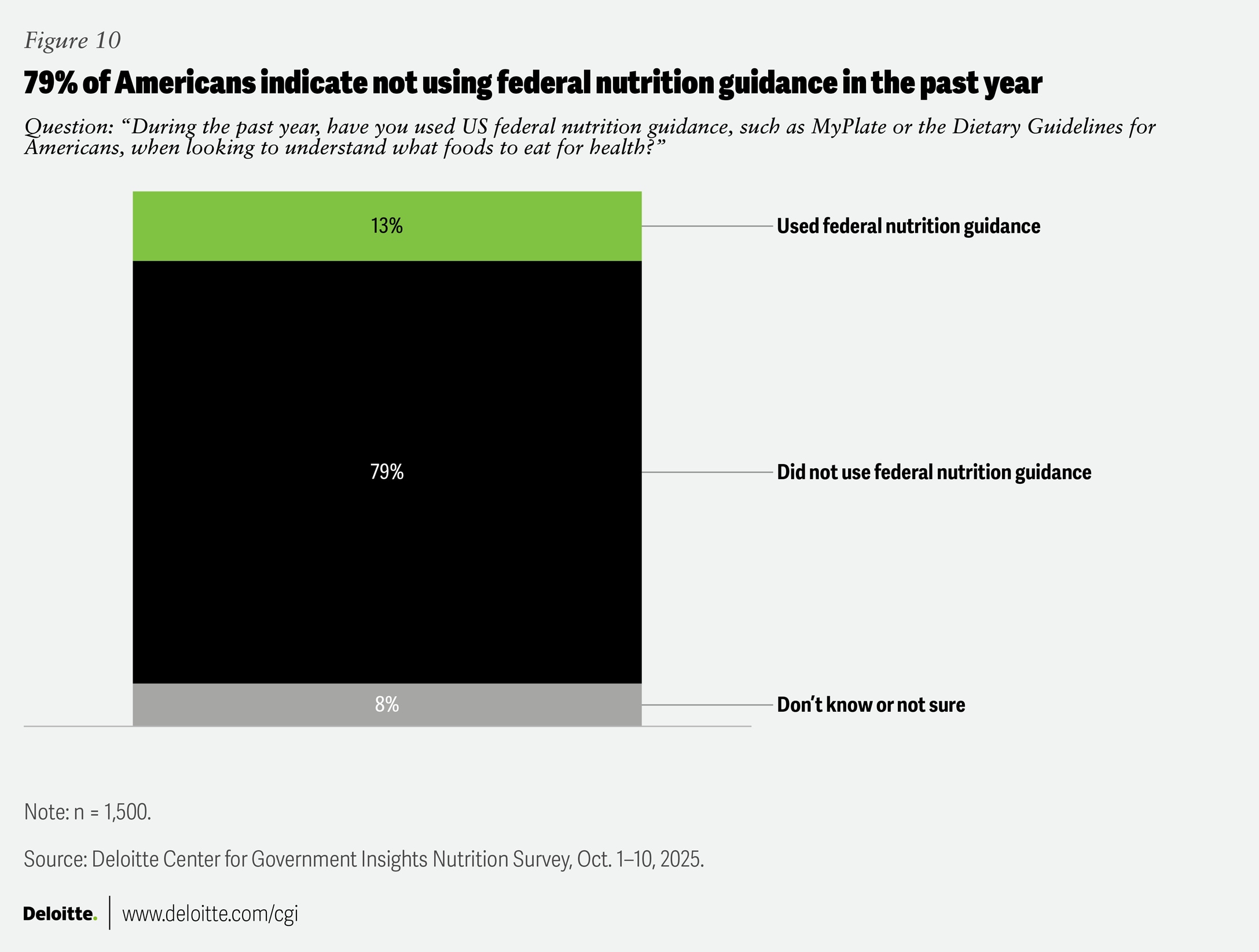
In contrast to the widespread use of nutrition labels, only 13% of respondents report using other federal resources in the past year, such as MyPlate, the visual guide for healthy eating—which was retired in January 2026, or the 2020–2025 Dietary Guidelines for Americans. Seventy-nine percent of respondents report not using these resources at all (figure 10). This low uptake points to an opportunity for the recently published 2025–2030 Dietary Guidelines—which are designed to promote healthy eating patterns and inform efforts to improve access to nutritious foods—to be translated into more digestible resources to support everyday decisions.17
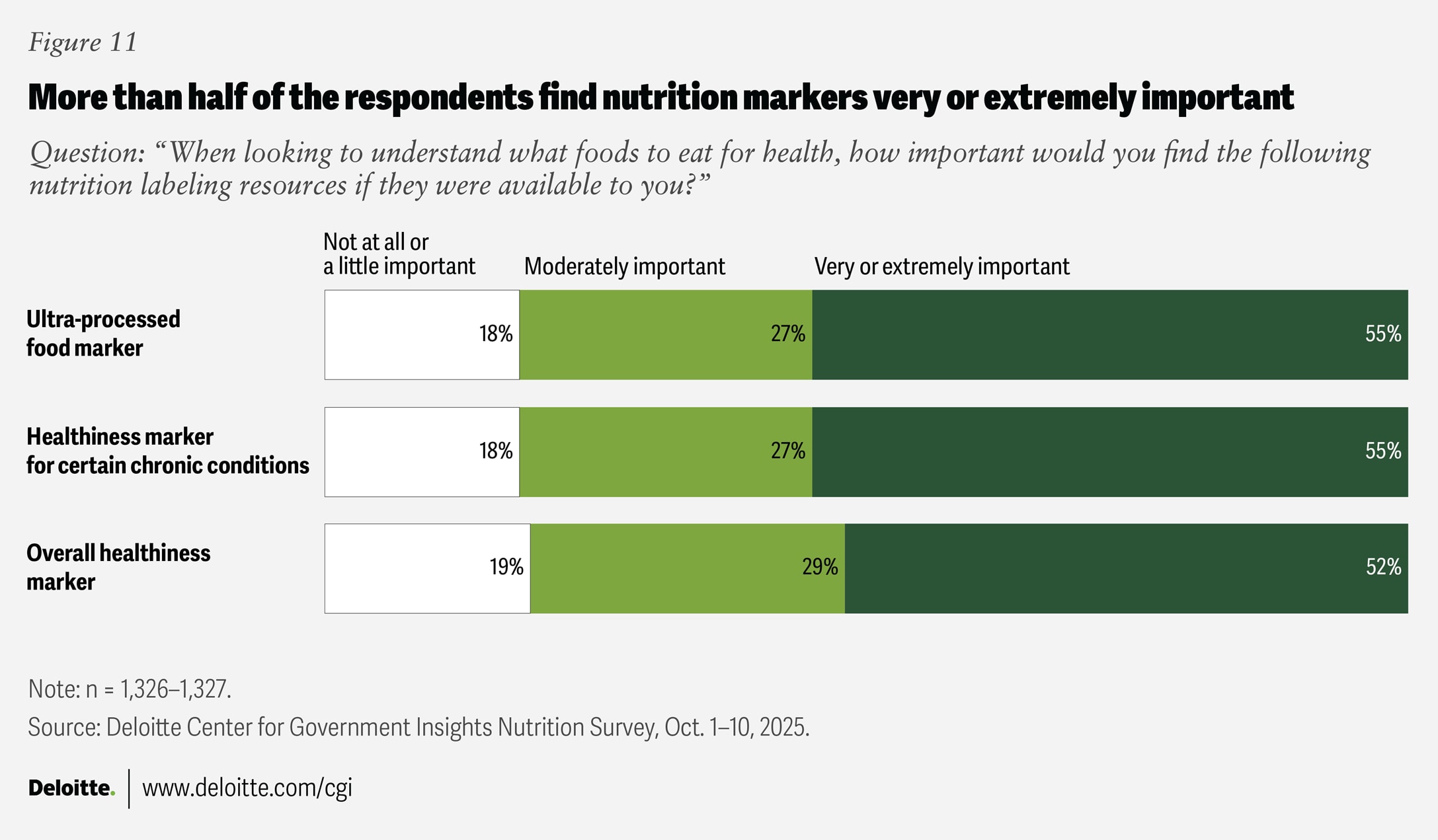
When it comes to understanding which foods to eat for health, respondents place high importance on three potential nutrition labeling tools: markers for ultra-processed foods, overall healthiness, and healthiness for specific chronic conditions. More than 50% rate each as very or extremely important, while about 20% consider them minimally or not at all important (figure 11).
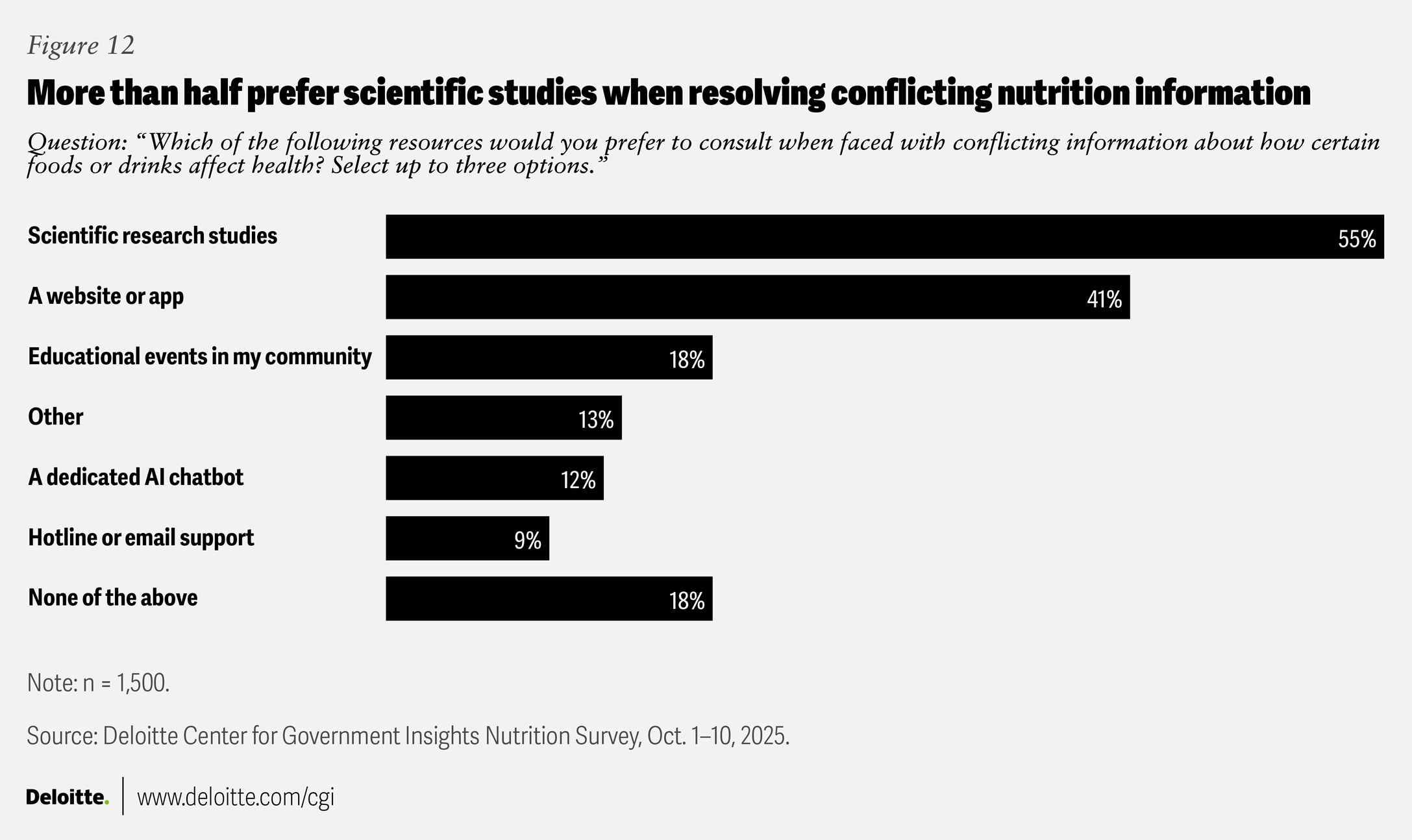
However, some respondents want to dig deeper and seek further explanations: Fifty-five percent say they would consult scientific studies to manage apparent conflicts in information (figure 12). This suggests that Americans may prioritize scientific evidence when questions or conflicts arise. Still, 41% say they would want a website or app to help them manage these conflicts, implying that easy access to information is also a priority.
When faced with contradictory nutrition information, our findings suggest that Americans want trusted interpretation, have an appetite for deeper understanding, and accept some uncertainty—as long as it’s clearly explained.
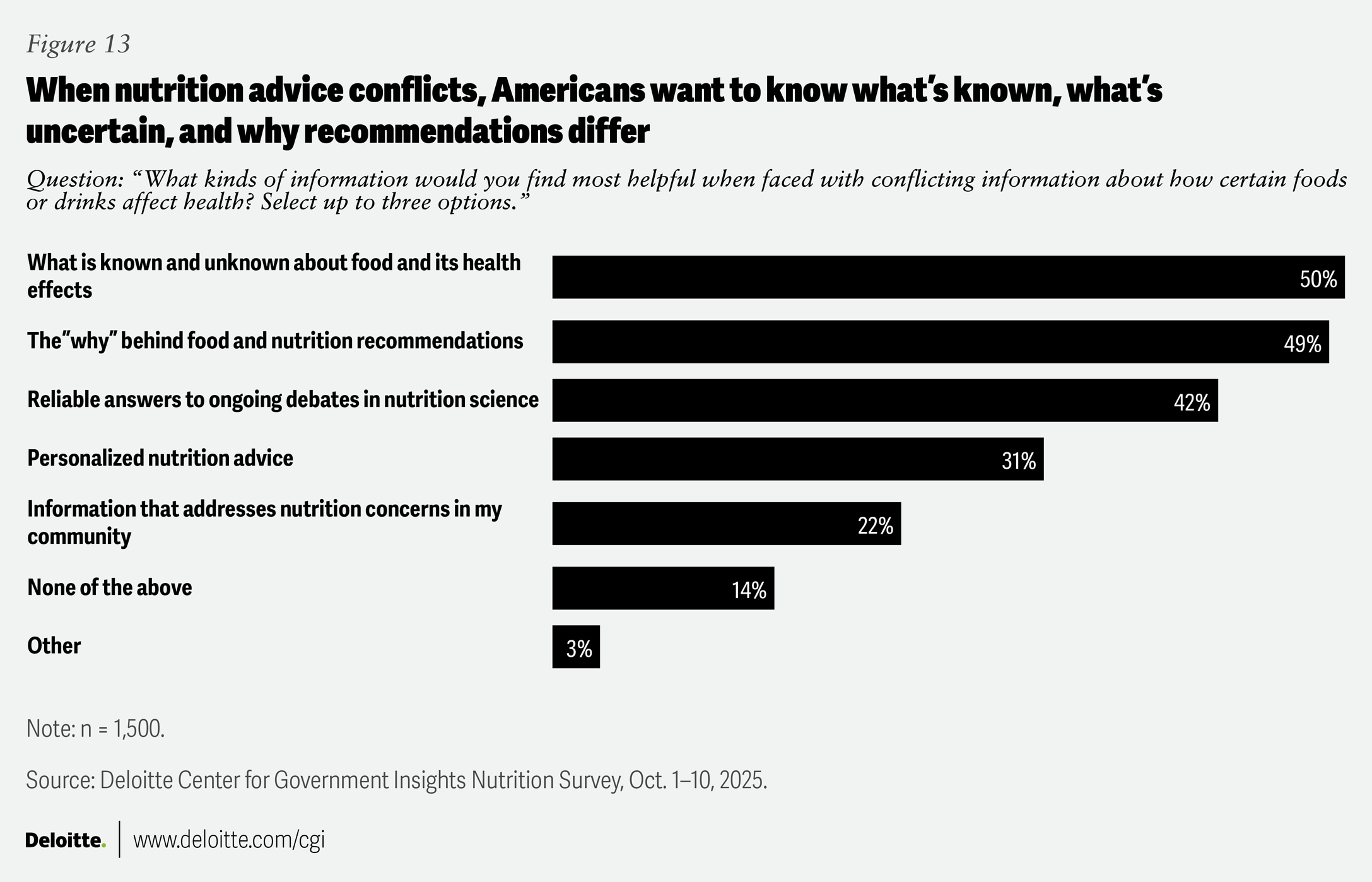
Americans may want scientific studies that can answer their top three information requirements (figure 13):
- What is known and unknown about food and its effects on health
- The “why” behind nutrition guidance
- Reliable answers to ongoing nutrition science debates
Still, 31% find personalized nutrition guidance most helpful, and 22% say information about nutritional needs specific to their communities would be most helpful.
Three considerations to make healthy choices easier
Our survey of 1,500 Americans shows that intuition and convenience often guide decisions about healthy eating. A confusing, sometimes conflicting information environment means that, despite prioritizing healthy eating, people may struggle to make healthy food choices.
More information alone likely won’t make people healthier, but making the healthy choice the easy choice can. Based on the survey results, we have identified three key considerations that can help Americans make healthier choices.
1. Clear and accessible nutrition labels could make nutrition information more widely understandable and usable. A majority of respondents felt that standardized markers for ultra-processed foods, an overall healthiness score, and healthiness scores tied to major chronic conditions would be helpful. Increasing the clarity and visibility of ultra-processed foods—by providing clear definitions and ultra-processed food-specific labeling on packaging—may help build public understanding.
Developing a widely accepted scientific standard for nutrition choices, especially for those with chronic conditions, may pave the way for providers to further incorporate nutrition information and guidance into traditional models of care. A shared, evidence-based framework for nutrition-related treatments, endorsed by government, scientists, and health care professionals, may also help insurers consider whether to cover such treatments in their plans.
Updating labels would involve coordination across the ecosystem, with government, retailers, food manufacturers, and others, to standardize “at-a-glance” signals at the point of purchase. Some grocery retailers have already implemented overall markers for healthiness to help shoppers make informed choices both in-store and online.18 One model uses a single score from 1 to 100 to signify the healthfulness of a food based on factors like nutrient density, while another store uses a star-ranking system to help customers distinguish overall item healthfulness.19
2. An ecosystem-driven, interoperable nutrition information hub could help Americans navigate conflicting messages and improve their eating habits. Our survey finds that respondents often feel confused by nutrition information and want clear labels and access to deeper resources to resolve conflicting information. A centralized hub, developed as a collaboration among federal agencies, nutrition scientists, retailers, and technology developers, could address these concerns by combining point-of-purchase guidance, scientific context, habit-building support, and personalized recommendations based on health needs, affordability, taste preferences, and demystified science.
Rather than replacing today’s tools, a centralized hub could establish common rails—data standards, labeling rules, and interoperability requirements—that private-sector innovators could build on. Recent advances in technology could make this vision for improving healthy eating across America more attainable.
To drive efficiency, the hub could build on existing efforts to advance AI-driven, interoperable medical records. By connecting with systems where people already receive care, a nutrition information hub could offer clinicians and patients alike nutrition data at the point of care. Within this platform, an AI-powered chatbot could also give Americans access to nutrition research from literature databases like PubMed in a digestible and easy-to-use format.
3. Well-crafted social marketing campaigns can shift behaviors, even among those with deeply entrenched unhealthy eating habits. Information alone has limited power to change eating habits;20 factors such as identity, emotions, social norms, and confidence in maintaining new behaviors can all influence food decisions.21 For this reason, social marketing campaigns can serve as a powerful complement to other efforts, helping achieve lasting dietary change by reshaping how people view food choices and everyday eating habits.
Healthy eating is important for reducing the overall chronic disease burden,22 yet many Americans struggle to meet recommended dietary guidelines. Evidence from past public health campaigns demonstrates the return on investment when campaigns are well designed and sustained over time. For example, the Truth Initiative’s “Know the truth, spread the truth” campaign featured real teens with opioid use disorders and emphasized that opioid dependence can happen in as little as five days.23 The campaign led to a 27% drop in the number of teens willing to share prescription opioids and a 600% increase in searches for the term “opioid epidemic.”24 Similarly, the Centers for Disease Control and Prevention’s “Tips from Former Smokers” campaign, which employed real stories of smoking-related harm from former smokers, has been associated with an estimated 16.4 million quit attempts and over one million sustained quits.25
These examples underscore the opportunity for modern nutrition campaigns to make a measurable impact. Leaders can consider reaching Americans where they most often seek information—across media and online environments, through health and science professionals, and within their communities (figure 6). Campaigns can also be delivered through libraries and local and state government resources, where our survey indicates respondents actively seek information at least twice as often as they encounter it by chance. By crafting campaigns that are entertaining, empowering, and relatable, modern nutrition campaigns could break through a crowded information environment, reinforce healthier dietary choices, and help shift everyday eating habits.
From confusion to clarity: Supporting Americans in making healthier choices
Every day, millions of Americans are making decisions about what to eat likely while scrolling, shopping, or cooking. Our survey of 1,500 Americans reveals that apparent conflicting information can make it difficult to know what counts as healthy, and many are uncertain about the health effects of processed foods.
While most respondents want to make healthier choices, many rely on gut feelings as much as nutrition labels and perceived health benefits when deciding what’s healthy.
To support these decisions, respondents want deeper context: explanations of why guidance exists and how evidence supports it. Making nutrition information easier to interpret, without oversimplifying, could help people navigate conflicting messages, build lasting healthy habits, and apply science in ways that fit their lives.
Clear labels, digital tools that help make sense of conflicting information, and engaging campaigns are ways to help Americans turn their intentions into healthy choices. The result could potentially be a future with less chronic disease for generations to come.
Methodology
The Deloitte Center for Government Insights conducted a cross-sectional online survey of 1,500 US adult residents of ages 18 years and older between Oct. 1 and Oct. 10, 2025.
The sample was nationally representative and weighted by 2024 presidential vote, age, sex, race, and education, with a margin of error of ±3.09%. Standard data quality checks were applied, including reviews of completion time and response completeness, and no respondents were dropped from the sample.
The aim of the study was to examine Americans’ perceptions, knowledge, and behaviors related to nutrition and healthy eating. Specifically, the survey explored how respondents define and prioritize “healthy” food; their understanding of ultra-processed foods; where they obtain nutrition information and how they navigate conflicting guidance; their use of food-as-medicine approaches and nutritional supplements; and their expectations regarding federal nutrition guidance, labeling, and programs.