Addressing root causes of health disparities across the globe.
Deloitte’s Health Equity Institutes help individuals fulfill their potential in all aspects of health and well-being.
“If you have your health, you have everything. When you do not have your health, nothing else matters at all.”
This insight from Augusten Burroughs holds true for all people, whether living in wealthy, mature countries or developing nations. Yet, for millions healthcare is unavailable, unreliable, or too costly. The result: poor health outcomes and untreated mental health challenges, along with diminishing trust in institutions.
Improving health equity is a multifaceted challenge, made more complicated because the social determinants of health vary significantly in their impact and include economic class, environmental effects and community investment in social services. Accepting that challenge and making progress toward health equity are integral to our humanity. Those realities are at the core of the Deloitte Health Equity Institutes (DHEI), which aim to improve health equity so that citizens can fulfil their human potential in all aspects of health and well-being.
Beyond infrastructure: Tackling root causes and contributing key capabilities
Health equity is about more than building health clinics, training health professionals, or shifting resources to where they are needed. It addresses the barriers that prevent people from living long, healthy and fulfilling lives.
The DHEIs, operating in Africa, India and the United States, collaborate with public, private and social sector organisations to explore and address three root causes of health inequity:
- Systemic bias, including racial, socio-economic and gender biases as well as others
- Disparate circumstances in the drivers of health, including factors such as income, adverse environmental conditions and lack of social support networks
- Inadequately designed, structurally flawed health systems, where lack of effective financing and infrastructure reduce access to primary health care services including screenings, drug coverage and mental health support
Teams in each DHEI show that these challenges are grave, but not insurmountable with the right capabilities and a flexible, methodical approach to problem-solving. As detailed here, each is developing long-term solutions to overcome the unique barriers to health equity within communities. Happily, the solutions and insights generated were immediately put to work and proven in initiatives that stemmed the tide of COVID-19 (see below).
Although Deloitte is not a healthcare organisation, through its DHEIs, Deloitte contributes three capabilities critical to understanding and solving the health equity puzzle:
- Action and Impact, through pro bono consulting with or in tandem along with financial support to community-based organisations who are working on health equity issues
- Knowledge and Evidence, by creating eminence, playbooks and insights to enable and influence others in our ecosystem to advance health equity; and
- Data and Analytics, by building analytical tools to generate actionable insights on health disparities
These capabilities, along with Deloitte’s global footprint, complement and enhance other organisations’ strengths and allow the DHEIs to transfer and scale solutions quickly.
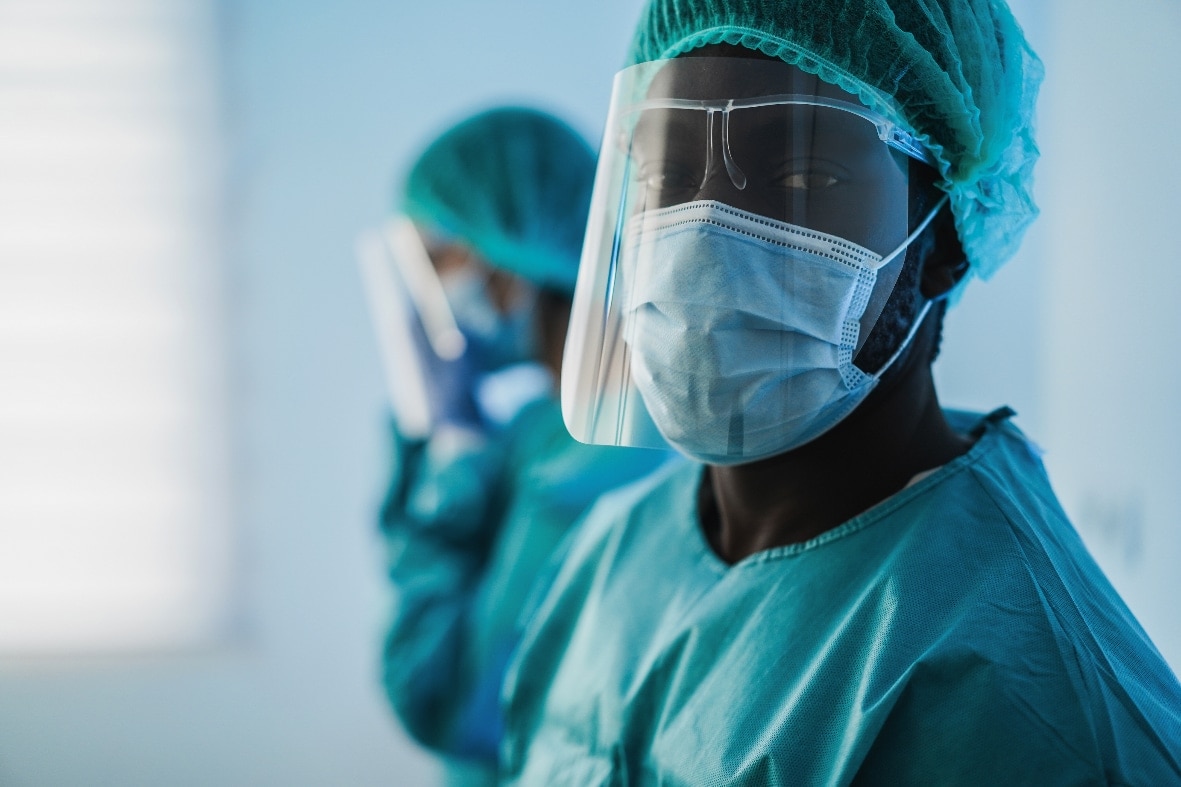
“By aggregating data on a range of topics to identify patterns, leaders are better able to target and deploy resources to underserved constituents and hot spots.”
Strengthening the mental health ecosystem in India
India’s mental health burden is enormous, doubling since 1990 and affecting an estimated 14 per cent of the population (200 million people). Yet, funding for treatment is minimal (< two per cent of the government health expenditure goes toward mental health) and the capacity of mental health professionals extremely limited (there are 0.07 psychologists or social workers per 100,000 citizens vs. >30 in the United States). These findings spurred India DHEI to action in this important area.
The team documented challenges faced by patients, policymakers, payors and providers by gathering insights about mental health from a mix of stakeholders (academics, to NGO leaders, to private and public providers). With facts in hand, the team identified six imperatives to address mental health inequities. These range from implementing and enforcing the current Mental Health Act and building digital treatment solutions, to focusing on and funding more community-based care. The goals: close the treatment gap, reduce the stigma of diagnosis and treatment, and minimise the years lived with disability (YLD). Acting on this concrete set of imperatives will reduce the economic loss of untreated mental health disorders in every Indian state and socioeconomic class, and fundamentally improve the lives of those who receive needed treatment.
Improving health care access through data sharing in Africa
The health equity disparities between urban and rural communities in Africa are large. Many countries face barriers to delivering basic health care services, particularly in rural regions. The problem is not only the lack of end-to-end infrastructure, but also gaps in resources. What’s needed is a seamless continuum of funding, proven programs and information flowing from national and district health agencies to communities and vice versa. Consequently, the Africa DHEI team focused on improving collaboration between health service organisations and increasing data exchange and transparency.
Effective efforts included conducting health equity workshops with policymakers in several countries, as well as fine-tuning a data analysis tool that captured relevant healthcare delivery data at the national, province, district and sub-district levels. By aggregating data on a range of topics that can be interrogated to identify patterns of illness, missed opportunities for treatment, or a falloff in health engagement, community and national leaders are better able to target and deploy resources to underserved constituents and hot spots.
Mitigating the health impact of poverty in US cities
In the richest country in the world, income level is still a major determinant of who receives adequate health care in the United States. At the root of inequities are historical mistreatment and bias, reflected across the country’s fragmented healthcare landscape. Indeed, many US citizens fend for themselves to get a diagnosis or treatment while others decline treatment available due to onerous costs, particularly for the uninsured. The result: many don’t trust or access services, even when encountering an existential threat like COVID-19, and acute conditions go untreated and lead to chronic disease.
The US DHEI invested in identifying and reaching low-income, underserved citizens. The team developed a comprehensive Health Equity Dashboard that generates granular insights of health equity in counties across the United States. Synthesising a range of credible big data sets, the dashboard’s advanced analytics help researchers and healthcare leaders visualise and understand the magnitude of health disparities, in large cities and small communities alike. As a result, insights generated help quantify relative risks for certain health conditions, like diabetes, that correlate to income, race, geography and age. Powered by Deloitte's HealthPrism Technology, the insights are available to the public—and health care providers and systems—for free, allowing targeted outreach to reach underserved populations.

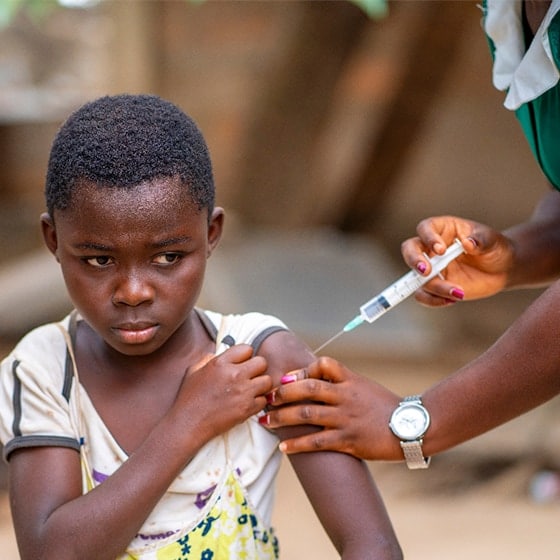

Deloitte Health Equity Institutes respond to COVID-19
Collaboration and information sharing are at the core of many DHEI initiatives, and both were deployed to improve COVID-19 health outcomes in targeted populations.
- Deloitte collaborated with leaders in India’s State of Haryana (Districts of Karnal and Rohtak) to implement a supervised, virtual, in-home care program that reduced strain on hospitals. This effort to “extend the hospital ward” served people in rural areas with mild or moderate symptoms by mobilising local healthcare practitioners and community-based workers to provide early detection (through home test kits), and essential care for home-isolated COVID-19 patients. Haryana’s technology infrastructure was used to establish a command centre to support higher acuity care. The successful approach was documented in a playbook, available across India and adaptable to other health crises. Learn more about the India Health Equity Institute
- Deloitte supported the South African government, Business for South Africa (B4SA), and other social partners and stakeholders to mobilise business resources and capacity to combat the COVID-19 pandemic. Deloitte created an end-to-end personal protective equipment (PPE) supply chain control-tower dashboard to generate a single view of PPE demand planning and procurement. The team’s efforts helped ensure the PPE supply to healthcare professionals during the crisis. Learn more about the Africa Health Equity Institute
- Teams across the country are collaborating with community organisations to build trust and improve access. In New York, the DHEI works with anti-poverty organisation Robin Hood to increase vaccination rates among difficult-to-reach populations. Together they fund health organisations that improve access to and reduce vaccine hesitancy grounded in misinformation, technology barriers and transportation gaps that exacerbate fear and distrust in the healthcare system. Similarly, in Washington D.C., Deloitte partners with the United Way of the National Capital Area, as well as the Choose Healthy Life Black Clergy Action Plan, to raise awareness and educate the Black community about COVID-19 and other health disparities. The US DHEI also invested in CommonSpirit Health’s outreach effort that engaged over 40,000 in rural Arkansas and California’s Central Coast. Learn more about the US Health Equity Institute
These are just a few of the ways the Deloitte Health Equity Institutes partner and invest to improve healthcare access and health equity for the world’s citizens. The DHEIs bring healthcare expertise, scalable solutions and tools, deep organisational development experience and, most important, passion and compassion to bear on the global problem of health inequity.
Learn more about the impact of our DHEIs.





